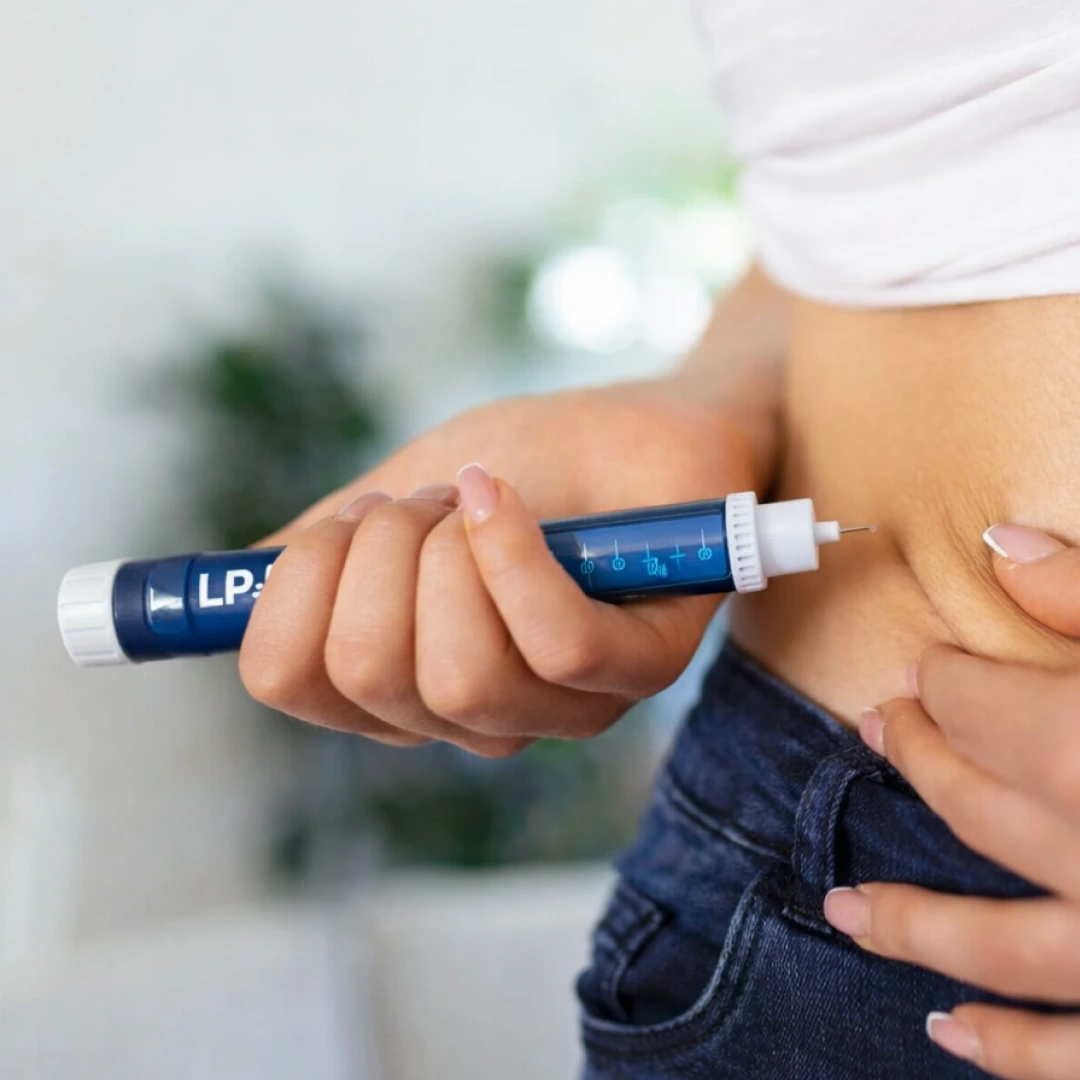
GLP-1 medicines (short for glucagon-like peptide-1 receptor agonists) are prescription drugs that can help with blood sugar control (in type 2 diabetes) and meaningful weight loss (in obesity management). Semaglutide is one of the best-known GLP-1s and is used in different brand/formulation contexts for diabetes and for chronic weight management.
But here’s the truth most people don’t hear clearly enough: GLP-1s aren’t “for everyone who wants to lose weight.” They are medical therapies with eligibility criteria, real side effects, and a list of people who should not take them.
This guide answers the most common “Am I eligible?” questions clearly, and with clinical guardrails.
Who should consider GLP-1 medicines?
You should consider GLP-1 medicines if you fall into one of these two buckets (and lifestyle changes alone aren’t getting you to a safe place):
1) Adults with obesity or overweight + health risks (weight management use)
Most clinical guidance and regulatory labelling align around this structure:
- BMI ≥ 30 (obesity), or
- BMI ≥ 27 (overweight) with at least one weight-related condition (examples: type 2 diabetes, hypertension, dyslipidemia, obstructive sleep apnea).
2) Adults with type 2 diabetes (diabetes use)
GLP-1s (including semaglutide) are widely used for type 2 diabetes, especially when weight, cardiovascular risk, or glucose control are key priorities.
Important: The exact “who qualifies” rules can vary by country, brand/formulation, and your personal medical history, so this is a decision to make with a clinician, not a checklist you self-approve.
What are the qualification criteria?
According to the FDA, think of qualification as 3 layers:
- Medical indication
- Weight management: BMI thresholds (above) ± comorbidities.
- Type 2 diabetes: clinician-confirmed diagnosis and treatment plan.
- Safety screen (contraindications + high-risk conditions)
- Thyroid cancer risk (MTC/MEN2), pancreatitis history, pregnancy, etc.
- Thyroid cancer risk (MTC/MEN2), pancreatitis history, pregnancy, etc.
- Readiness + monitoring
- Ability to follow dose escalation, manage GI side effects, stay hydrated, and do follow-ups (weight, symptoms, labs if needed).
Is this only for people with diabetes?
No. GLP-1 medicines were first used broadly in diabetes care, but some GLP-1s (including semaglutide in certain formulations) are also indicated for chronic weight management in adults who meet BMI criteria.
Can I take it if I’m overweight but not diabetic?
Possibly, if you meet the BMI + comorbidity criteria.
If you’re:
- BMI ≥ 30 → you may qualify even without diabetes.
- BMI 27–29.9 → you usually need at least one weight-related condition (like high BP, high cholesterol, sleep apnea, prediabetes, etc.).
If your BMI is below these ranges, many clinicians will first focus on lifestyle, nutrition, sleep, strength training, and addressing drivers like insulin resistance, because risk/benefit may not justify medication.
What BMI or weight do I need to qualify?
Most evidence-based obesity pharmacotherapy criteria commonly used:
- BMI ≥ 30, or
- BMI ≥ 27 with a weight-related comorbidity
Why BMI isn’t the whole story:
BMI doesn’t show visceral fat, fatty liver risk, glucose variability, or cardiometabolic risk. That’s why clinicians also look at waist circumference, labs (HbA1c, lipids), blood pressure, sleep, liver markers, and overall risk profile.
Can women take GLP-1s? Can men take GLP-1s?
Yes, GLP-1s are used in both women and men, and eligibility is based on medical need + safety, not gender.
Where sex-specific nuance matters is mostly around:
- Pregnancy planning/contraception
- PCOS and fertility changes
- Side effect tolerance (some people experience nausea more intensely)
Is it safe for older adults?
Older adults can use GLP-1s, but they require more careful monitoring, especially for:
- Dehydration risk from nausea/vomiting/diarrhoea (which can affect the kidneys)
- Frailty or low muscle mass (rapid weight loss without resistance training can worsen sarcopenia)
- Polypharmacy and appetite changes (risk of under-eating protein)
Age alone isn’t an automatic “no”, but the plan should be more medically supervised.
Can I take it if I have PCOS?
Sometimes, yes, but this is often an “off-label” discussion, depending on your country and the exact product indication.
Why it can come up in PCOS:
- Many people with PCOS struggle with insulin resistance, weight gain, and appetite dysregulation.
- Weight loss can improve cycles, metabolic markers, and symptoms for some.
What to do:
- A clinician should evaluate your metabolic profile (glucose, lipids), goals, and pregnancy plans.
- If you’re actively trying to conceive, GLP-1 use typically becomes a “pause and reassess” conversation.
Can I take it if I have thyroid issues?
It depends on which thyroid issue.
If you have hypothyroidism / Hashimoto’s:
That’s not the same as the thyroid cancer risk in GLP-1 boxed warnings. Many patients with hypothyroidism use GLP-1s under supervision.
If you have a personal/family history of medullary thyroid carcinoma (MTC) or MEN2, it is a hard stop:
- GLP-1 medicines like semaglutide (per labelling) are contraindicated in people with a personal or family history of MTC or MEN2.
If you’re unsure what type of thyroid condition you have, don’t guess; ask your clinician to clarify your diagnosis.
Who should absolutely NOT take GLP-1s?
According to the FDA, GLP-1s are generally not appropriate (or require very strict specialist oversight) for people with:
- Personal or family history of MTC (medullary thyroid carcinoma) or MEN2
- Pregnancy (and generally not recommended while planning pregnancy). Discuss timelines with your clinician.
- Serious hypersensitivity to semaglutide or product components (rare, but in labelling)
And caution/avoidance is commonly discussed in people with:
Is it safe if I have kidney problems?
Often yes, but with important caution.
Semaglutide labelling notes no dose adjustment may be needed in renal impairment; however, there are post-marketing reports of acute kidney injury, often linked to dehydration from GI side effects.
Translation: kidneys aren’t usually the direct problem; dehydration is.
If you have kidney disease:
- Your clinician may monitor renal function more closely,
- You’ll need a clear hydration plan, and
- You should report persistent vomiting/diarrhoea early.
Is it safe if I have liver issues?
Many people with metabolic conditions also have fatty liver. In general, semaglutide does not require dose adjustment for hepatic impairment per labelling, but “safe for liver issues” depends on what liver issue you have and how advanced it is.
If you have:
- Mild to moderate fatty liver → This is a common scenario clinicians evaluate in metabolic care.
- Advanced liver disease/cirrhosis → requires specialist management.
Can I take it if I had gallstones before?
GLP-1 therapies can be associated with gallbladder issues in some people, and rapid weight loss itself is also a known gallstone risk. If you’ve had gallstones before, it’s not always an automatic “no,” but it’s a strong “proceed carefully” category.
What “careful” means:
- You should know the warning signs (right upper abdominal pain, fever, jaundice),
- Escalate symptoms early,
- And ensure weight loss is not too nutritionally aggressive.
Can I take it if I have pancreatitis?
This is one of the most important red-flag topics.
Pancreatitis is listed as a potential risk with GLP-1 medicines, and regulators continue to monitor it. People with a history of pancreatitis often require specialist decision-making (and may be advised to avoid).
If you develop severe abdominal pain (especially radiating to the back), nausea, vomiting, or fever, seek medical attention promptly.
Is it safe if I plan to get pregnant?
In general, GLP-1 medicines are not recommended during pregnancy, and planning pregnancy should be discussed before starting. The key issue is fetal safety and the need to stop the medication in advance based on the product’s pharmacology and labelling guidance. (FDA Access Data)
If pregnancy is on your horizon:
- Tell your clinician upfront.
- Ask for a timeline-based plan (stop date, alternative strategies, metabolic optimisation).
Can I take it while breastfeeding?
Breastfeeding is another “needs clinician input” category. Many medication labels take a cautious stance because data may be limited or because risk/benefit depends on the situation. Treat this as a do-not-self-prescribe zone; get a clear medical recommendation. (FDA Access Data)
So… how do you decide the right fit?
If you want a simple, responsible way to decide, use this framework:
You might be a good candidate if:
- You meet BMI criteria (≥ 30, or ≥ 27+ comorbidity)
- OR you have type 2 diabetes, where GLP-1 is clinically appropriate
- You don’t have the key contraindications (MTC/MEN2, pregnancy, etc.)
- You can commit to medical supervision and side-effect management.
According to the FDA, you should avoid or pause until medical review if:
- You have a personal/family history of MTC or MEN2
- You’re pregnant, actively trying, or breastfeeding (without explicit medical clearance)
- You have a history of pancreatitis, or you develop symptoms suggestive of it
A practical “next step” checklist (what to ask your clinician)
Bring these to your consult:
- Your goal: diabetes control, weight loss, PCOS/insulin resistance support, or cardiometabolic risk reduction
- Your numbers: BMI, waist, BP, HbA1c, lipids, liver enzymes, kidney function
- Your history: gallstones, pancreatitis, thyroid cancer/MEN2, pregnancy plans
- Your plan for sustainability: protein + strength training + sleep + follow-up schedule
- Your monitoring: symptom tracking and hydration plan (especially during dose escalation)
Where GoodFlip can fit in (even with a “general POV”)
GLP-1 medicines work best when they’re part of a full metabolic system, labs, habit change, coaching, and tracking, because the goal isn’t just “lighter,” it’s metabolically healthier over time. That’s also why platforms like GoodFlip focus on combining diagnostics + coaching + smart tracking into a single journey (and not treating weight as the only outcome).